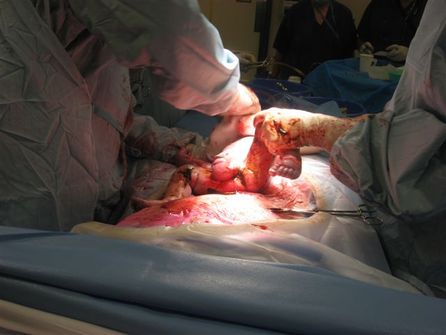
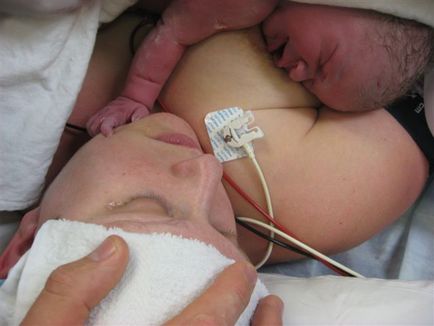
 Thank you Hannah for sharing your birth story with us. You can read about Hannah's encapsulation experience after her c-section too VBAC turned CBAC for all the “right” reasons On 8 January 2013 the stars collided. Once again, a beautiful baby entered my world to change my life forever. Hamish Joel was born via an emergency caesarean. It was not the entry I had dreamed of but his birth was a powerful and empowering event. The story of Hamish's amazing journey earthside however starts with an outline of his sister's birth 20 months earlier. Bethany Grace was born via emergency caesarean after 21 hours of labour. An unneccaesarean due to her posterior presentation & Failure to be Patient (FTP) on the part of conservative care providers. Prior to Bethany's birth I thought I was educated. I did the yoga, read the literature, did an active birth workshop, had a student mid-wife, did “shared care” because I didn't get into the birth centre. Heck I wrote an 8 page birth plan. Boy was I wrong! My pregnancy with Bethany was complicated. After a threatened miscarriage & following lack of support from my workplace I had an emotional breakdown, was diagnosed with perinatal anxiety & depression & placed on medication. Sure I did yoga but I succumbed to emotional eating, put on lots of weight and stopped my regular exercise regime. I experienced a huge disconnect in my care provision at the end of my pregnancy whereby I was given a late diagnosis of GD (Gestational Diabetes) at my 36 week clinic appointment with a dragon of a midwife who announced in no uncertain terms how incompetent she thought my GP was. I was then given the scare tactics of the “big baby” card by a well meaning OB. Bethany's labour was unproductive. I arrived at hospital to only be 4cms. Rather than go home I stayed certain I would progress quickly due to the timing of the contractions. Not one of my care providers had told me prior to her labour that she was posterior presentation. Not my GP, the midwife who was so horrid, or even the “experienced” OB who I saw after the nightmare diagnosis of GD. She hadn't switched or moved. She had been in the same spot since 25 weeks gestation. Not one of the three midwives who attended me during the labour told me they thought she might be posterior. I firmly believe had I been given this vital piece of information her delivery may have been different. But at the time I didn't know any better & I bought the crap of the OB who delivered her that it was the safest means for her to come into the world as she was “distressed”. What baby in distress comes out with an APGAR score of 9 though? I asked myself this & many many other questions after her birth. I doubted my ability to birth babies, I felt broken & cheated of the natural vaginal birth I had worked so hard for. I mourned what I didn't get & was determined that next time it would be different! Next time it would be a vaginal birth or if surgery was required it would be for the right reasons. Next time I would see my child enter the world. Next time I would be the first to hold my child & not have them whisked away from me for three hours. Next time it would be different. My husband & I had always discussed our children being close in age & even before Hamish's conception I had started my VBAC journey. When the pregnancy test came back positive I put the wheels in motion to make my pregnancy the most healthy & to maximise my chances of a VBAC. I had already lost the weight gained in Bethany's pregnancy & post-partum period. I read everything I could get my hands on, birth stories, books. I questioned everyone to find out their experiences with care providers. I continued to exercise doing RPM , weight lifting & vinyasa yoga up to 32 weeks. After this I walked every day & continued my prenatal yoga up to delivery. I watched my diet diligently & whilst I declined the GTT & GTC I monitored my own blood sugar levels. I got myself an awesome doula. I ensured continuity of care by taking the steps I needed to in order to be accepted into a VBAC friendly publicly funded birth centre. I quizzed my midwife, built myself a support team, & advocated for myself at the hospital to decline interventions that protocol would otherwise decree I must have as a VBAC mumma. I refused the routine group & save on admission, canulla & continuous monitoring. I wanted & gained support to be able to labour & deliver in water. I did Spinning Babies inversions daily & hassled my midwife every single visit after 27 weeks about my baby's position. Most importantly I worked on my head space. I felt that in Bethany's labour I “overthinked” the whole thing. I knew that for me to get my VBAC I needed to let go. I needed to trust my body to do what it was built to do. I needed to relinquish “control” & tap into the primordial part of my brain, the animalistic part that enables us to birth babies. For this I enrolled hubby, doula & myself in a hypnobirthing course. Following on from which I listened to my tape & practiced my relaxation daily. I also discussed my fears openly with my husband, doula, midwife & close friends. In doing this I gained the support I needed to feel safe. Everyone in my team knew our birth plan. I would stay at home as long as possible, essentially rocking up at hospital to push. If I was 5cms dilated or less on admission I would go home. I was determined to VBAC but not at all costs. I knew there were some real circumstances within which a caesarean would be necessary & worked hard to feel at peace with these circumstances should this be an outcome. Hamish was LOA/LOT from about 27 weeks gestation. He moved a little from time to time but was essentially in the optimum foetal position leading up to the night before his birth at 39 +3 gestation. On this night lying in bed before going to sleep I joked with my husband about putting towels in the bed& our brand new car should my waters break. Little did I know that only a few hours later, at 1.31am to be precise, my waters would not only break but gush with the force of Niagra Falls in the bed & all over the bedroom floor. My waters were clear & I informed the hospital when I rang them that I intended to go back to bed to rest. I was told to re-contact if anything changed otherwise I would hear from my midwife the following day. I went back to bed & within 45 minutes felt the twinges often described as period pain-like. Within 2-3 hours these twinges were real surges that I would work through every 8 minutes or so but I laboured peacefully in bed. Listening to my hypnobirthing CD I closed my eyes & whilst I didn't sleep felt quite rested. I used my breath to work through the surges & let them wash over me. My doula Trish & mum arrived at 6.30am. By the time they arrived my surges were 3 minutes apart. I had spoken with my midwife who had told me to let their length build up further as they were only 20-30 seconds in duration. Shortly after Mum & Trish arrived the surges increased in duration & maintained their 3 minute breaks between. In hindsight it was as if my body had permission to let go once I knew my little princess was being looked after & I had the gentle female support that only a doula can provide. I told my husband James to contact my midwife & speak to her. She told him that we could stay at home longer if we wished but it sounded like I was making fantastic progress. My doula knew otherwise though & said to James that if we wanted to make the journey to hospital (& contend with peak hour traffic) we would need to look at moving shortly. She knew how much I wanted to use water & gently guided me to the shower. Not long after we made the journey to the hospital by car. Trish was an absolute godsend for this 45minute to 1 hour journey. She was my rock & my soft place to fall. Her presence enabled James to focus on the journey & me to focus on staying internal, in my birthy zone. Trish & I were both in the back seat of the car. I was in a bizzare all fours position. Right hand holding onto the handle above the window, left hand pushed into the back behind the car-seats & feet pushing downwards into the floor of the car. I had my eyes firmly shut the entire time & a cool flannel over my head. Trish supported me if we went around corners or James had to brake suddenly. She flicked the air-vents on if I barked out “HOT”, off if I barked “COLD” & placed her warm hands in the right spots to apply firm counter-pressure for my ever-widening hips. Without her I would have lost it- she was truly amazing. When we arrived at the hospital a midwife greeted us in the Emergency ramp with a wheel chair that I not so politely declined. The usual protocol was for us to go into the Women's Assessment Service (WAS) a holding pen of sorts to determine if I was far enough progressed to go up into the delivery suite. I worked through several surges on the way to WAS & on entry was told I could be “taken straight up”. Apparently the noises I was making were enough of a give-away that I was well & truly in labour land. On the way up to the 3rd floor I found great relief in hanging of anything I could. Similarly to in the car, as soon as a surge hit I would look for something to hang off & drop into a squat of sorts. Almost like a monkey in a tree hanging from branch to branch. Apparently this got some interesting looks when the lift stopped at every floor, James also assures me that we got some great looks during the car ride in. When we arrived at the labour ward I was told that the room I had did not have a bath to which I not so politely stated “I want a room with a bath, now”. Some swift moves meant I got a room with a bath & Trish got to work running it as soon as we went into the room. I went into the toilet where I sat on the toilet & hung off the rails during my surges. It was here that I had a conversation with my midwife. She asked me how I was feeling to which I answered “great, this feels so much more different to Bethany's labour, productive, intense but good, I'm feeling pushy”. I told her I could feel my hips widening & the baby dropping down. She praised my efforts & told me that she could see how well I was working with my surges. She told me she was happy to leave me to see how things went or if I wanted I could have an internal. I elected to have the internal as I wanted to be sure that I should be in the hospital. My midwife did the internal & announced “great news you are 6 cms” then paused “but that's not a head”. She told me that she was going to have to call the doctors in. I instantly knew what this meant, baby was breech, I would have surgery, & I went into shock. Breech vaginal deliveries are a rarity let alone in the hospital environment. Being a VBAC mumma was an added “hindrance” to breech being considered a variation of normal. All of this I knew but I also knew that I was determined to have a breech vaginal birth if that was at all possible. The first doctor I saw was a young, conservative female. She did an ultrasound to confirm Hamish's breech presentation then touted previous section, previous big baby as reasons to section immediately. I requested a second opinion all whilst shaking from what I thought was just shock. It is at this point I should mention that we arrived at the hospital at roughly 8.30am& Hamish was born at 10.10am. I was transitioning & in shock about the prospects of another surgical birth. On my request for a second opinion the female doctor brought the head consult into the room & reiterated her reasons for cutting me- breech big baby in a VBAC mumma. The consult, who I will hereafter refer to as Dr C, asked her how she knew baby was big. Its no surprise her answer was she didn't know! Dr C then assumed the lead role. He looked at baby Hamish on ultrasound & conducted an internal examination. He confirmed that Hamish was in fact breech & told me that not only was the baby breech but a footling breech. With all my prior reading & research I knew this was a highly risky position. There is a 15-30% increased risk of cord prolapse & most scarily a significantly high chance that once the feet & torso are birthed the cervix shuts down on the neck leaving baby trapped. Both of these are very emergent situations & I knew that if anything like this was to occur this would result in me being knocked out under a general anaesthetic. It would also likely lead to my baby going to the neonatal ward. The female doctor asked me “what was I so afraid of with a section”.Ha! Full abdominal surgery lady! I have a toddler at home to care for- what do you think I am afraid of? Silly woman had no idea! But I was equally afraid of my baby unduly suffering for my zealous quest for a VBAC. I didn't want my baby to have to be resussed. I didn't want my baby going to neonatal. I didn't want my baby to have a fractured pelvis or shoulder. I didn't want to be knocked out. I wanted to be present & available for my baby who I wanted to hold immediately & not be separated from. I looked to Trish & told her “I have no choice” to which she said “yes hon you have a choice. You can choose when this happens & have some control or you can let things go the way they will”. I pleaded with my husband to make the decision for me. He told me he knew how much the VBAC meant to me & that if we consented he knew I would still regret it. He told me he didn't want to make the final decision & that whilst our baby's health was paramount it was truly up to me. I knew consenting to the section earlier was going to optimise my ability for me to watch the birth & have immediate skin-2-skin contact with my baby. So I consented but on my terms. I told them I would only sign for the section if I could watch the birth, have baby given straight to me & examined on my chest. The Paediatrician met with me before we went to theatre & assured me that if baby came out ok all of these things would occur. Once I signed the consent & as I was feeling very pushy I asked for some gas. I decided that if I was going in for surgery then I might as well be comfortable now because there was no way I was going to get my bath! The trip down the corridors to theatre was the worst part, I knew where I was going & what was going to happen. I knew that I was going to be cut again & was spontaneously pushing. When we arrived in theatre Dr C told me he knew how much a VBAC meant to me. He stated that as I had progressed so beautifully, I was now at 10 cms, if the baby tucked their feet up then he wanted me to “push that baby out my vagina”. With my permission he gave me another internal to see if the baby's feet were still dangling, they were & little Hamish had descended significantly down the birth canal. Dr C then called the surgery & within 20 minutes my spinal was in & Hamish was out. The drapes were lowered, James saw everything & even over my belly I was able to see two legs emerge out of my stomach. James announced we were having a boy! Little Hamish cried & pooped all over Dr C who used my own language from my birth plan to explain how the baby would come straight to me. After a quick glance without even a single rub down Hamish was placed naked on my chest. True skin-2-skin, no wrapping up in blankets with only his head poking out but instead naked, birthy goop & all! James & I were truly over-joyed! My student midwife took some amazing pictures of Hamish's entrance earthside & helped him latch within 10 minutes. And lets just say since he discovered the breast he's never wanted to leave it! On reflection a few things strike me as truly amazing. My body worked! It went from waters breaking to fully dilated & pushing within 9 hours! I wasn't broken! While I went to a very primal place I was able to be lucid & articulate when I needed to in order to get the best care available to me. An experienced OB gave me every opportunity in the world to have a safe vaginal delivery & recognised the importance of a VBAC. Heck he even used my own language from my birth plan& told me that he wanted me to push this baby out of my vagina! The power of true support & a birth team plus quality care results in good birth outcomes. Hamish's birth was a surgical birth but it was dramatically different to Bethany's. It was empowered & it was supported by medical evidence. It was necessary. I owned it. I had choices. Yes I could have let nature run its course but I know that nothing on this earth would ever let me forgive myself if something had have happened to Hamish purely out of my “quest” for the redemption I believed a VBAC would bring me. In the haze of newborn sleep deprivation, a prolonged recovery due to a second operation to re-suture, being house-bound & feeling worthless as a mother to my toddler I have questioned Hamish's birth. I've played the “what if I didn't get that internal” card round & round in my head. But as I've physically healed I've returned to a place whereby I am empowered & emotionally healed by Hamish's birth. He entered earthside surgically but safe& for the right reasons. The risks were too high. My body was amazing, did all the right things & I was not separated from my darling little man. I found my redemption & know that I am not broken. I am a birth warrior! Read about Hannah's experience with placenta encapsulation
Flik
6/4/2013 04:35:09 pm
What an incredible story Hannah. You have shown that it IS possible to have control over our births- as is our human right- even in a hospital setting and under circumstances that the overwhelming majority of medical professionals on this country would sadly consider high risk. You fought the good fight towards VBAC- you armed yourself with knowledge, you gathered an amazing support crew, you were conscious and proactive throughout your pregnancy, you laboured naturally and COMPLETELY... And YOU did ALL of this whilst growing a baby and mothering a toddler! I am so inspired by your strength and power. Thank you for sharing your amazing story. X
Hannah
10/4/2013 09:08:27 am
Thank you Flik <3
Debbie
23/4/2013 12:59:24 pm
You did the right thing, Hannah. So glad the senior ob helped make the birth a better experience for you. If I end up with another c for my next birth, I want to be fully present at the birth like you were. You are such a strong person and don't forget that. Some natural birth advocates say that great personal growth comes only from natural birth and that's wrong. When we accept the c sections we don't want, we are abandoning our own desires and just "doing what we have to do" as parents - there's incredible personal growth from the experience. Thank you, thank you, thank you!!!! Just over 5 month ago I was truly on my way to have an amazing Hypnobirth only to end up in an emergency c-section. And to add not only that, my boy was for 5 days in the special care. I thought I came to terms with it, only to have a breakdown today when I heard what an amazing birth my friend had yesterday. All these feelings of uselessness, guilt and self blame where back. Thank you for sharing your story so that I can realise what I experienced wasn't planned but nothing short of amazing. Comments are closed.
|
freebiesPrepare for an easier fourth trimester with these 25 Secrets From A Postnatal Doula!
blogs
All
About MeKelly Harper is the owner of Elemental Beginnings Doula & Placenta Services in Adelaide. She provides sleep consultancy, placenta encapsulation and doula services to families during pregnancy, birth and in their fourth trimester. |
|
© 2024 Elemental Beginnings |
|
PREGNANCY, BIRTH & POSTNATAL SUPPORT DELIVERED WITH ❤ THROUGHOUT ADELAIDE & SURROUNDS